
- 2 Comments
- PRMA Plastic Surgery
Recently, Dr. Chrysopoulo and breast cancer survivor Erika sat down to discuss the impact of radiation on breast reconstruction. We covered a lot during the Facebook LIVE event and we don’t want anyone to miss out on the valuable information discussed. Check out the replay below or read more on the hot topics discussed below.
What type of reconstruction is recommended when radiation is planned?
There are many options for breast reconstruction available today. When radiation is planned, breast reconstruction using your own tissue is strongly preferred instead of implants for many reasons. At PRMA, we believe the DIEP flap is today’s gold standard for breast reconstruction.
What are the benefits of tissue (or autologous) reconstruction after radiation?
With autologous reconstruction, a soft, warm and natural breast is created. All damaged tissue is removed and replaced with healthy tissue from the donor site. The results look and “feel” like a natural breast. Sensory nerve reconstruction can also be performed to help patients regain more sensation following the mastectomy.
When tissue expanders and implants are used, the damaged radiated skin cannot be replaced but instead has to be stretched. Unfortunately, the radiated skin can become quite firm and very often does not stretch well. This increases the risk of complications – when radiation is in the mix, almost 1 in 3 implant reconstructions fail and the patient is left without a breast. Flap procedures like the DIEP flap have a much higher success rate, over 99% in fact at PRMA
When is the best timing for breast reconstruction after radiation?
Many reconstructive surgeons prefer to delay breast reconstruction when radiation is part of the treatment plan. Most patients are told they should wait 6 months to a year before proceeding with reconstruction. However, at PRMA we have found undergoing tissue-based reconstruction with a flap as early as 6 weeks after radiation is safe. In fact, for some patients it is preferred. The longer a patient waits to undergo reconstruction after radiation, the greater the amount of scarring that can develop. By performing a flap reconstruction sooner, we interrupt the scarring process early on by re-introducing healthy tissue to create a warm, soft breast.
Immediate DIEP flap breast reconstruction (at the same time as the mastectomy) can still be performed if radiation is planned, however, a coordinated team approach involving a radiation oncologist experienced in treating breast reconstruction patients is key in decreasing the risk of complications.
What if a patient finds out they need radiation during a mastectomy with immediate DIEP flap reconstruction?
This is not an ideal situation, but there are options. One option is to proceed with reconstruction then refer to a radiologist who has extensive experience in radiating DIEP flap patients. Another option is to place a tissue expander to get the patient through the radiation therapy while preserving as much of the breast shape as possible. The tissue expander can then be replaced with the DIEP flap after radiation is completed. This staged approach is known as “delayed-immediate” reconstruction. It is important to ask your surgical team about their protocol in this situation before surgery.
Can implants be removed and replaced with DIEP flap after radiation?
Absolutely! Patients who are unhappy with their previous implant reconstructions frequently come to PRMA for this very reason.
If a male breast cancer patient undergoes radiation, what breast reconstruction options are available?
Fat grafting is the most common form of breast reconstruction for men. After radiation, fat grafting would still be recommended, but it may take more than one procedure to achieve optimal results. In extreme cases, flap procedures can be performed to replace the damaged radiated tissue with healthy, soft tissue, usually from the back (latissimus flap).
Remember you are your own best advocate! It is important to discuss all your options with your surgical team and through shared decision making decide what is best for you.
Author: Dr. Minas Chrysopoulo and Courtney Floyd
Miss the LIVE event? No worries! Catch the replay here!
Leave Comment

I had nipple sparing with expanders then radiation. Had failed implant. I’m wondering if i will have to lose nipple if I do diep. The breast shrunk and is up high
Liz horton
October 23,2020

Your surgeon should take every precaution to save the nipple during reconstruction surgery, but it is never a guarantee that the nipple can be saved.
PRMA Plastic Surgery
October 27,2020
Sign Up for Our Monthly Newsletter
Continue Reading

Breast Reconstruction Surgery and Your Period
Breast Reconstruction Surgery and Your Period December 02, 2020 Share on Facebook Twitter Linkedin During our pre-operative appointment with patients, a topic that occasionally arises is menstrual cycles. It is completely normal for women to experience changes with their periods throughout breast cancer treatments. These can be temporary or permanent. Periods can be unpredictable following […]

What Bras and Abdominal Girdles to Wear After Breast Reconstruction Surgery
What Bras and Abdominal Girdles to Wear After Breast Reconstruction Surgery November 17, 2020 Share on Facebook Twitter Linkedin When preparing for breast reconstruction surgery, many patients want to know what types of bras and abdominal girdles they should plan to wear after surgery. Although every surgeon has slightly different preferences, we have put together […]

My 5 DIEP Flap Realities | A Guest Blog From Julie
My 5 DIEP Flap Realities October 28, 2020 Share on Facebook Twitter Linkedin Hi everyone, my name is Julie from It’s a Bosom Thing. I am so happy to be here as a guest blogger and have this opportunity to share with you a few thoughts about life after DIEP Flap Surgery. I was diagnosed […]

PRMA’s BRA Day Virtual Event Recap
PRMA’s BRA Day Virtual Event Recap September 08, 2020 Share on Facebook Twitter Linkedin Yesterday we celebrated Breast Reconstruction Awareness day! Although we missed seeing everyone in person this year, we were still able to spread education and awareness on ALL reconstructive options through our virtual efforts. We were also able to share information on […]
Second Stage DIEP Flap Surgery
Second Stage DIEP Flap Surgery September 08, 2020 Share on Facebook Twitter Linkedin DIEP flap breast reconstruction is typically comprised of at least two stages for the best outcomes. The second stage of surgery is commonly referred to as the “revision” stage and is usually performed about three months after the initial reconstruction. The purpose […]

If ‘Flaps’ Are Such A Great Breast Reconstruction Option, Why Doesn’t Everyone Get Them?
If ‘Flaps’ Are Such A Great Breast Reconstruction Option, Why Doesn’t Everyone Get Them? September 08, 2020 Share on Facebook Twitter Linkedin Flap-based breast reconstruction procedures, like the DIEP flap, offer patients a safe, natural implant-alternative option to reconstruction after a mastectomy. Flap surgeries are permanent and are associated with fewer complications after radiation when […]

What is a Skin Island and How is it Used in Breast Reconstruction?
What is a Skin Island and How is it Used in Breast Reconstruction? September 08, 2020 Share on Facebook Twitter Linkedin What is a “skin island”? The term “skin island” is used to describe the remaining visible skin from a transplanted “flap” of tissue. In the setting of DIEP flap breast reconstruction, the skin island […]
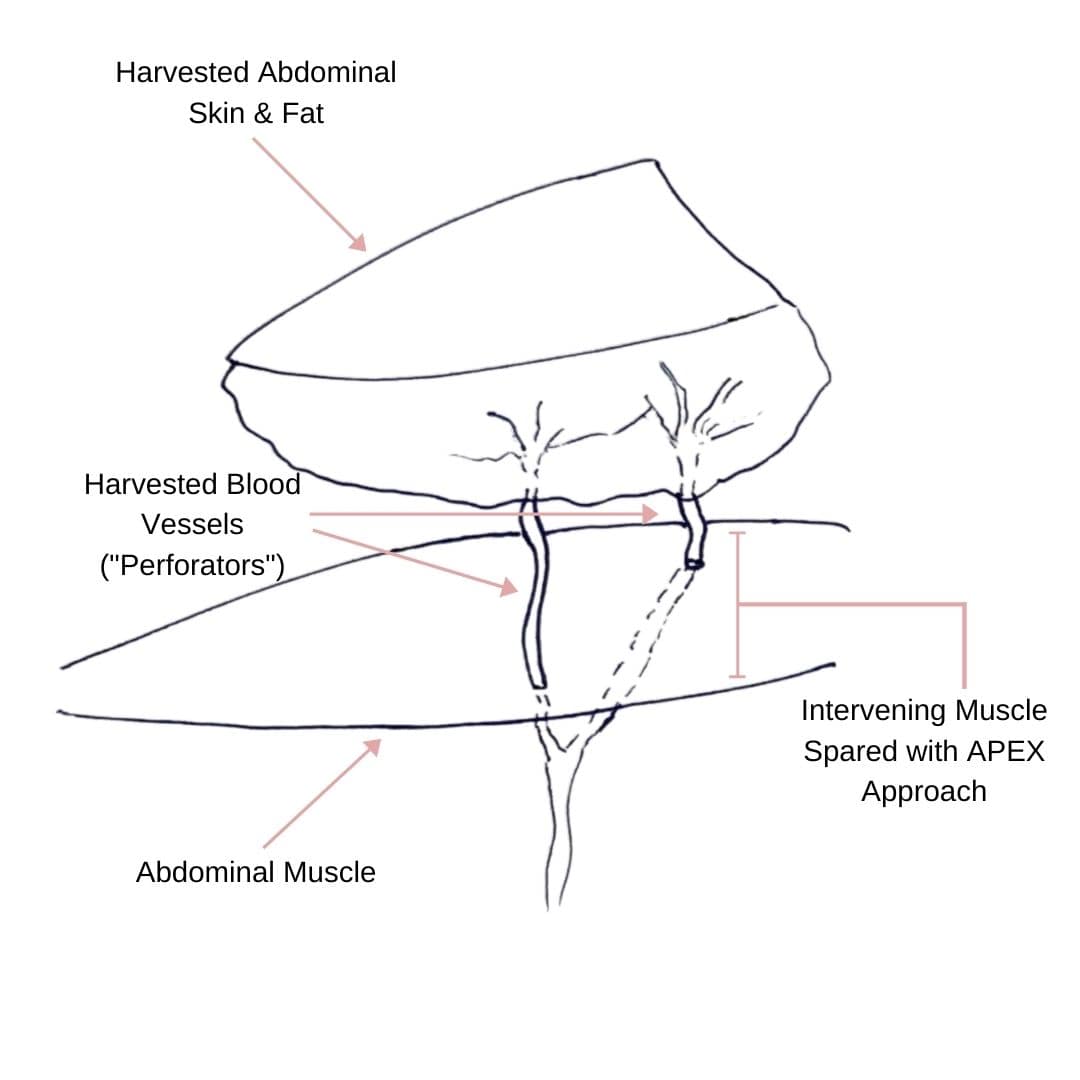
Comparing APEX Flap and DIEP Flap Breast Reconstruction
Comparing APEX Flap and DIEP Flap Breast Reconstruction August 10, 2020 Share on Facebook Twitter Linkedin We have been receiving numerous inquiries about the “APEX flap” recently. Patients want to know what it is and how it differs from the DIEP flap. APEX is an acronym that stands for “Abdominal Perforator Exchange”. Many patients believe […]
Monitoring the Health of Your Flap During & After Surgery
Monitoring the Health of Your Flap During & After Surgery July 21, 2020 Share on Facebook Twitter Linkedin Autologous flap (or tissue) breast reconstruction procedures represent today’s most advanced options for rebuilding a breast(s) following mastectomy. The most commonly performed method of flap-based reconstruction at PRMA is the DIEP flap. During this procedure, surgeons transplant skin […]
COVID-19 and the Impact on Cancer Patient’s Mortality
COVID-19 and the Impact on Cancer Patient’s Mortality July 21, 2020 Share on Facebook Twitter Linkedin There is still so much we do not know about COVID-19. Likewise, there is little known about how this disease impacts mortality for cancer patients. A study published in The Lancet evaluated and characterized the outcomes of patients with cancer […]
Capsular Contracture Part Three: Treatment
Some Patients No Longer Required by Insurance to Wait for Breast Reconstruction

Liz horton
I had nipple sparing with expanders then radiation. Had failed implant. I’m wondering if i will have to lose nipple if I do diep. The breast shrunk and is up high
PRMA Plastic Surgery
Your surgeon should take every precaution to save the nipple during reconstruction surgery, but it is never a guarantee that the nipple can be saved.